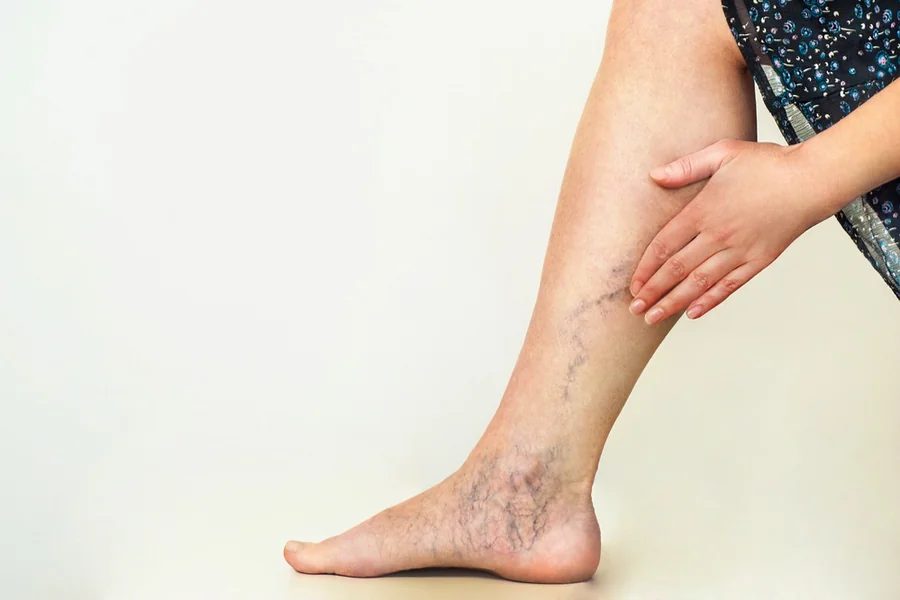
Varicose veins are enlarged, twisted veins, often visible on the legs, that occur when blood doesn’t flow properly and begins to pool. While many people think varicose veins are only a cosmetic issue, they can actually indicate underlying circulation problems and may cause discomfort, heaviness, swelling, and pain.
Understanding the leading causes of varicose veins can help you identify risk factors early, seek proper care, and prevent complications. In this blog, we will understand what exactly varicose veins are and explore the leading causes of varicose veins.
What are Varicose Veins?
Veins carry blood back to the heart through a system of one-way valves. These valves open to allow blood to move upward and close to prevent it from flowing backwards. When the valves weaken or the vein walls stretch, blood may begin to pool rather than circulate efficiently. This creates pressure, causing veins to bulge and twist, which can lead to varicose veins.
They most commonly appear on the legs and feet because standing and walking increase pressure on the veins in the lower body. At the same time, although not always dangerous, untreated varicose veins can lead to complications such as swelling, skin discolouration, dryness, itching, and, in severe cases, venous ulcers.
Main Causes of Varicose Veins
Varicose veins can develop for several reasons. Some causes are lifestyle-related, while others are genetic or structural. Below are some causes:
1. Weak or damaged vein valves
The most direct cause of varicose veins is faulty valves inside the veins. When these valves fail to close properly, blood flows backwards and accumulates in the vein. Over time, the vein becomes enlarged, twisted, and visible through the skin. This valve malfunction can be due to age-related wear and tear, chronic inflammation, or even prolonged pressure on the veins. Once valves are damaged, they rarely return to normal function without medical intervention.
2. Ageing
Age is one of the most significant risk factors. As we get older, our veins naturally lose elasticity and become more fragile. The valves inside them also weaken, making it harder for blood to flow upward. Most people start noticing early signs of varicose veins between the ages of 40 and 50. Age-related changes include thinning of vein walls, reduced muscle tone, and stiffening of tissues supporting the veins.
3. Genetics and family history
If your parents or grandparents have varicose veins, your risk increases significantly. Genetics influence the strength of your vein walls and the functionality of your valves. Inherited traits may include weak connective tissue, valve abnormalities, and higher pressure in the leg veins. This one cannot be controlled, but early awareness and the correct varicose veins treatment help with prevention.
4. Pregnancy
Pregnancy is a common trigger for varicose veins due to several physiological changes. Some physiological changes include increased blood volume, hormonal shifts, and increased pressure from the uterus. While some pregnancy-related varicose veins improve after childbirth, many women experience long-term vein dilation.
5. Prolonged standing or sitting
Your job or lifestyle can significantly influence vein health. When you stand or sit for long periods, the calf muscles, which help pump blood upward, remain inactive. This allows blood to pool in the lower legs. Lack of movement increases pressure in the leg veins, which can eventually lead to valve failure.
Conclusion
Varicose veins develop due to a combination of weakened valves, genetic factors, age, hormonal influences, and lifestyle habits. While some causes, such as family history or ageing, cannot be avoided, many others can be managed with better movement, weight control, and early medical evaluation. Understanding what leads to varicose veins will help you take preventive steps and seek timely care. In more advanced cases, specialists may explore minimally invasive procedures or even vascular surgery to relieve symptoms, improve circulation, and prevent long-term complications.